TL;DR
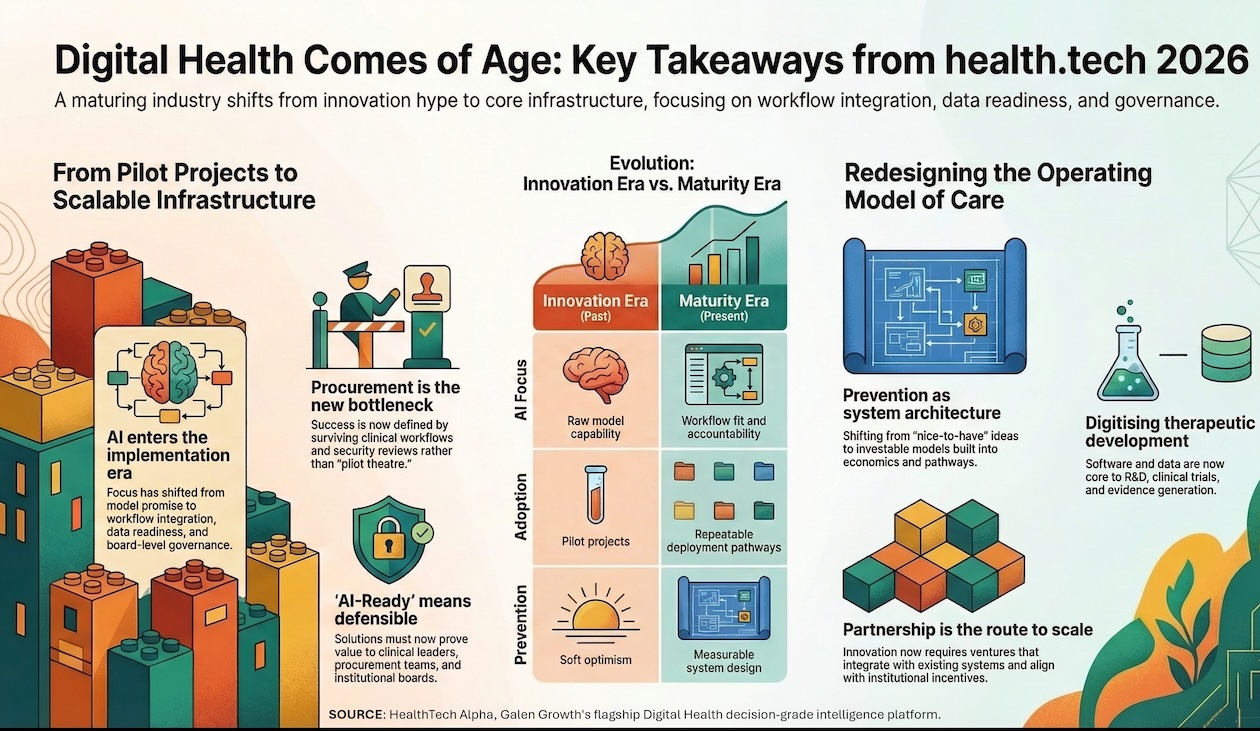
- AI has entered the implementation era: the market now prioritises workflow integration, data readiness, and governance over abstract model promise.
- Adoption remains the bottleneck: procurement, risk management, and operational ownership are still where pilots stall—or scale.
- Prevention is maturing into systems design: early detection and personal health are shifting from rhetoric to operating-model questions.
- Therapeutic development is being digitised: trials, endpoints, evidence generation, and R&D execution are becoming increasingly software- and data-led.
- Galen Growth showed up as a signal engine: from Investor Speed Dating to clinical trials thought leadership to the booth’s “Digital Health” buzzword board, the focus was on turning conference energy into durable intelligence.
Last week in Basel, the health.tech global summit made something unmistakably clear: Digital Health is no longer being discussed as a peripheral innovation theme. It is increasingly treated as core infrastructure—and the industry is entering a new phase of digital health implementation.
The conference programme reflected that shift with unusual discipline. Rather than trying to be everything to everyone, health.tech concentrated around four substantive tracks:
- next-generation therapeutic development
- preventive and personal health
- modernising the mechanics of care
- AI in healthcare
The result wasn’t a parade of futuristic claims. It was a more mature conversation—one that increasingly asks not “what’s possible?” but “what scales?”
Basel is a fitting place for that shift. In Europe’s life sciences capital, ambition tends to meet reality quickly. That intersection—between vision and execution—was the defining energy of the week.
AI has entered the implementation era—and “AI readiness” is becoming a board topic
The first major theme was unmistakable: AI in healthcare has moved from novelty to necessity, and from experimentation to deployment. The language around AI has tightened. Less fascination with raw model capability; more scrutiny on what it takes to embed intelligence into real systems.
Across sessions and conversations, the implied criteria for AI success were consistent: workflow fit, data integrity, governance, explainability, and accountability. AI is no longer treated as a product feature. It is becoming a board-level capability—because scaling AI in healthcare inevitably touches compliance, risk, safety, ethics, and institutional trust.
A telling adjacent signal of that mindset was the emphasis on creating environments for real-world experimentation and co-innovation—explicitly designed to shorten the distance between AI ambition and operational deployment.
Adoption is still the bottleneck—and procurement is finally being treated as a first-order problem
If there is a single “hard truth” that continued to surface this week, it is this: adoption remains Digital Health’s choke point.
The ecosystem has learned the limits of pilot theatre. Many solutions can demonstrate value in a controlled environment. Far fewer can survive procurement cycles, clinical workflow constraints, integration complexity, security reviews, budget realities, and governance structures.
What felt different in Basel was how directly this friction was discussed. Procurement, risk management, and operational ownership were not treated as afterthoughts or “later-stage” issues. They were treated as first-order determinants of whether innovation becomes infrastructure.
This is the maturity marker the market has needed: shifting prestige from pilots to repeatable deployment pathways.
Prevention is moving from “nice idea” to systems design
Prevention and personal health were present not as soft optimism, but as system architecture. The questions were less about whether prevention matters—and more about how it becomes real: early detection, longitudinal data, risk stratification, engagement models, and the incentives that determine who acts and who pays.
That shift is important. Prevention has historically been an aspiration with weak operational scaffolding. The stronger framing emerging now is that prevention is an investable model only when it is built into pathways, economics, accountability, and measurable outcomes.
In Basel, the tone was less sentimental. More pragmatic. And ultimately, more credible.
Digital is reshaping therapeutic development—not just downstream care
The week also reinforced a structural reality: the boundary between “digital health” and “biopharma” is eroding.
Therapeutic development is becoming increasingly data-led and software-mediated—from discovery tooling to clinical-trial recruitment, decentralised execution, endpoints, evidence generation, and post-market insights. The conversation is no longer whether digital belongs in R&D. It is how fast organisations can operationalise it responsibly—and how quickly the ecosystem can align around evidence standards and regulation.
The implication is clear: digital is no longer an add-on to therapeutics. It is becoming part of the operating system.
What participant commentary added: less theatre, more execution—with Basel’s personality intact
A good conference has two agendas: the official one and the one expressed in hallways, side events, and LinkedIn posts. The latter was unusually consistent this week. Across founders, investors, corporates, and health-system participants, three themes kept surfacing.
First, the market is no longer impressed by abstract AI promise; the question now is whether a solution actually works inside real workflows, reduces friction, and earns adoption.
Second, evidence, governance, and data quality are moving from background concerns to centre stage, with participants repeatedly signalling that “AI-ready” now means being defensible to clinical leaders, procurement teams, and the board.
Third, partnership is increasingly becoming the only credible route to scale: healthcare innovation is less and less about lone disruptors and more about ventures that can integrate with the existing system, align with institutional incentives, and build trust across stakeholders.
And then there was the now-famous wine fountain—a recurring motif in attendee commentary that captured the spirit of the week rather well: serious conversations, serious ambition, but without taking the industry’s own theatre too seriously.
Galen Growth’s contributions: turning conference energy into durable signal
Against that backdrop, Galen Growth’s footprint this week mapped directly onto the summit’s strongest themes: execution, decision-support, and adoption.
Investor Speed Dating: making capital allocation more signal-driven
By helping power high-velocity investor-startup engagement, Galen Growth reinforced a simple truth: capital allocation remains one of the cleanest signals in Digital Health. Curated interaction isn’t just networking. It is real-time discovery—who gets attention, why, and what patterns are emerging across investor theses and startup positioning.
Thought leadership on clinical trials: clearing a bottleneck that still defines the industry
The session on digital tools for faster, fairer trials landed squarely in the conference’s implementation mood. Clinical trials remain a critical constraint on timelines and cost. Digital approaches—AI-enabled feasibility, smarter recruitment, decentralised infrastructure, and more efficient execution—are now judged by whether they measurably compress cycle times, improve inclusion, and de-risk delivery. The framing also pointed to the real unlocks: targeted investment, regulatory alignment, and cross-ecosystem collaboration.
The booth as a signal engine: “Digital Health” defined in public
The Galen Growth booth did something most booths don’t: it invited the ecosystem to define “Digital Health” in their own words. The Digital Health buzzword board turned the booth walls into a live market-sensing surface—participants sharing viewpoints, challenging language, and surfacing what they believe matters now: outcomes, workflow, evidence, interoperability, reimbursement, trust.
That wasn’t decoration. It was a reminder of a deeper truth: Digital Health isn’t one thing, and the market’s definition is evolving. Capturing that evolution—what terms are being retired, what’s being reclaimed, and where stakeholders disagree—is itself intelligence.
Don’t just inspire—equip
Finally, making HealthTech Alpha accessible through the conference app reinforced a practical philosophy: conferences generate momentum, but decision-makers need a system of record once they return to their desks. In a higher-scrutiny era, decision-grade intelligence—coverage, comparables, evidence signals, partnership mapping—becomes more valuable, not less.
The takeaway: the market is growing up
The deeper takeaway from health.tech Basel 2026 is this: the Digital Health market is becoming more serious.
Serious about data quality and governance. Serious about workflow integration. Serious about procurement and adoption. Serious about regulation and trust. Serious about prevention as a system design problem. Serious about the convergence of digital with therapeutic development.
For startups, the implication is clear: novelty is not enough. For corporates: waiting is no longer a strategy. For investors: opportunity remains abundant, but only for those who can separate scalable infrastructure from presentation-layer promise.
Basel didn’t just host a conference this week.
It hosted the Digital Health ecosystem in execution mode.